Modernising the Social Model in Mental Health: a discussion paper
Foreword
We are living in truly interesting times. The Government's new look at health policy contains some pleasant as well as potentially nasty surprises for proponents of the social model. Many who had experienced the 1980s and 1990s as increasingly hostile to social science and social approaches looked to the Government of 1997 to usher in a new dawn. However, scrutiny of health policy as it emerges reveals a number of inherent contradictions and tensions. These may yet mean that social approaches, social work and social care services - and critically, social science research - retain their Cinderella status in both the public imagination and in the focus and orientation of new structures for the commissioning and delivery of services. Recent articles in both the Health Services Journal and Community Care attest to increasing anxiety about the future amongst social workers and an emerging recognition of the negative impact of several years bad press. The Observer of September 16th 2001 led with a statement from the Association of Directors of Social Services about an impending meltdown in child protection services unless urgent action is taken to increase morale and to recruit more staff. More recently, the Secretary of State has announced a recruitment campaign aimed at addressing an escalating crisis in social work recruitment and retention whilst, at the same time, ‘naming and shaming’ a number of low performing departments of social services. There appear to be contradictory messages about the value of the social model and its place in modernising health policy.
Nowhere is this tension more apparent than in the mental health field, where the publication of the National Service Framework (NSF) has provided a framework for the development of comprehensive, integrated, user-focused services requiring high level, multi disciplinary skills. Moreover, the framework provided by the NSF acknowledges the need to not only develop effective services to adults with mental ill health but to prevent it in the first place. This connects the new mental health agenda to the radical new agenda for public health established by Saving Lives: Our Healthier Nation, the English public health white paper, which emphasises the multi factorial nature of population health and well being. The understanding that health is to a large extent socially and economically constructed has particular relevance for tackling health inequalities and for the development of wide ranging interventions aimed at tackling the root causes of poor health in communities and individuals. The strategy has ushered in a range of new initiatives aiming to improve health, many of these, including health and other Action Zones and Sure Start operationalise a social model of health and emphasise the need for community development and empowerment as both a means and an end in health improvement. Significantly, Sure Start is a Treasury led and funded initiative.
However, at the same time, new health policy is increasingly dominated what have been called ' scientific- bureaucratic approaches' such as clinical governance that emphasise the validity of certain kinds of 'hard' scientific investigation and intervention over others. The NHS Plan in England and equivalents in Wales and Scotland have been criticised by many analysts for being overly focused on the health of the NHS rather than the health of the population.
The recent report of the Health Select Committee notes this potential tension when it states:
' We accept the Secretary of State's assurance that the NHS Plan is of equal status to Saving Lives. We particularly welcome the fact that the Plan includes a commitment to health inequality targets. But we believe that a great opportunity has been lost by the lack of emphasis in this area of the Plan……. We believe that it adds credence to the notion that, for all the laudable Government rhetoric about dragging public health out of the ghetto, in the race for resources, it runs the risk of trailing behind fix and mend medical services. '
This difficulty in sustaining the focus on public health is not surprising given the history and the strength of the dominant medical template within which we conceptualise notions of health and sickness, structure our services and direct our investment. These systems require that services achieve outcomes for their users that relate to targets established by high- status, scientific approaches rather than those that are driven by local and individual needs and wishes. In support of this agenda, clinicians have been placed in the driving seat of the new NHS structures. The development of Care Trusts which will provide seamless support to vulnerable groups of people are viewed by many within the NHS as an extension of the territory currently governed by PCTs and by local government as a potential loss of power and influence - and an erosion of local democracy. This has fuelled fears that there will be a lack of understanding or appreciation within the new NHS of the value of social approaches - or that these will be understood only as the practical support provided through social care services and annexed to NHS-led interventions as a subordinate, lower status element. There are particular concerns that without the support, however frail, of departments of social services, social work will be unable to retain its distinctive profile or assert the value of its contribution in mental health and other areas of services and will, as a result, be lost.
These suspicions are particularly intense in mental health where proposals to reform the Mental Health Act have generated widespread concerns about the implications for human rights and, it is feared, will undermine the professional autonomy of social workers. Indeed, examination of emerging mental health policy suggests that the thrust of developments within the field are more focused on the safety of the general public rather than the empowerment of mental health service users and the prevention of poor mental health within communities. This is markedly at variance with the health policy messages from other sectors - and particularly from public health.
This paper considers the new policy environment and explores both threats and opportunities for the social model. However, it rests on the premise that if we look beyond the field of mental health, notwithstanding a range of tensions and conflicts, current developments in public policy may be the best opportunity we have had in several decades to assert the value of the social model. However, this will not happen by default. If this potential is to be realised there is need for clarity about the nature of 'the social', new definitions of practice, greater connectedness to the evidence base, renewed attention to the skills and value base of those who provide social interventions and to the measurement of their impact. The continuation of confident and assertive forms of social work is vital to the endeavour. This is vital if the profile of the model is to be retained within an increasingly multi disciplinary service context.
Modern mental health policy suffers in the same way as all earlier policy regimes from severe difficulty in relating macro to micro preoccupations. In short, we see this in the glaring absence of real people, of evidence of a grasp of the lived experience of patients, carers or even professionals, in policy documents and the thinking which drives them. The commitment to service user participation is present as a consistent, but in the end qualitatively empty commitment within the whole culture of current mental health policy. To be afflicted with mental health difficulties, means amongst other things to suffer at a subjective and social level. In turn, this means that those caring for and living with users often suffer with and on behalf of them. But in policy terms the story is rarely narrated from this perspective, and is consigned to the domain of ‘clinical experience’ or research into users’ lives. We know from user research that people want mental health interventions above all in the form of consistent relationships with professionals, and that counselling and talking therapies are also highly valued. Talking in the context of structured relationships is in itself one kind of ‘social model’ of mental health work, and we neglect this basic insight at our peril.
Our policy cultures are no stronger at producing meaningful thought about the nature of relationships than they are with respect to subjectivity and experience. The rhetoric of ‘partnership’ tends to be good at thinking about how any two categories of stakeholder might join or collaborate, but often functions in an exclusionary manner when three or more enter the picture. The contributions of managers and users are valorised at the expense of the contribution of the professional, or commissioners and users at the expense of the provider, and so on. The struggle with the reality of complexity in policy and practice relationships is still in its infancy, although there are encouraging signs that this is changing in a number of recent NHS Confederation briefings.
For legitimate and important reasons associated with the traditional concept of what it is to be a professional, clinicians and practitioners have had a hard time at the hands of government and the structures supporting their collective autonomy have been challenged and subjected to scrutiny. But users value good professional work,and do not want to see those responsible for their care devalued or undermined. The project of representing the experience of professionals as well as those of users and carers in the service of promoting policy thinking and strategy which truly connects the micro with the macro – the simultaneous individual, group and social dimensions of lived experience - and breathes life into policy prescriptions and action from this stance, is one of the central aims of the Social Perspectives Network for Modern Mental Health (SPN) which this document has played an important role in bringing into being.
Maria Duggan
Andrew Cooper
Care management has meant the loss of my skills. The ability to be creative is gone. It has been about brokering packages of support on behalf of my client, not about advocating for them, empowering them and their networks, helping them to understand and cope with their illness. Relationship is no longer possible in any therapeutic sense. I am prevented by the way the service works from my using my skills to actively engage and to sustain the engagement over time. This is what I was called to do and trained to do. I haven't researched this , but my observation is that relapse is more frequent amongst clients now, the despair is greater as we have retreated from the preventive role. My links with the CMHT have been entirely to do with arranging social care assessments. I am leaving next week to do a Masters Degree in creative writing because I cannot continue to work in this way .
Mental Health social worker. Department of social services. London
Purpose
This paper considers emerging mental health policy in relation to the overall modernisation agenda in health, social care and other public services. Whilst noting a number of contradictions and tensions in the policy field, it suggests that these developments provide a vital opportunity to articulate and implement a social model of health and to promote new forms of practice aimed at promoting community and individual empowerment. Consideration is given to the evidence base for such approaches generally, and in relation to mental health. Examples of practice based on the model are provided within the paper.
The paper considers the nature of the social model in the modernised policy context. It suggests that this is a model that emphasises the complexity of health and illness within individuals and communities and which therefore opens the door for multiple strategies for intervention, drawing on the expertise of a range of different disciplines and agencies. The model is rooted in an understanding of the impact of power and powerlessness on health. It considers an increasing body of evidence that suggests that individuals suffer poorer health, both physical and mental, if they live in more unequal places. The raw correlations that are sometimes found are increasingly viewed as the result of factors other than income inequality and are intimately linked to broader notions of inequality and unfairness. In taking account of this evidence the paper asserts that the model understands the importance of the quality of interaction between the individual and his or her social context for both physical and mental health. It is therefore a social model that engages with the inner worlds and lived experiences of individuals and communities as well as with external social, economic and environmental factors.
The model proposed in this paper does not struggle for domination with the medical model but urges greater synergy based on greater awareness of what works - and when. However, this approach needs organisational support if it is to be effective and will require new skills and new understandings amongst mental health workers. There is cause for some concern that developing structures for commissioning and providing mental health services, driven by tight, centrally-controlled performance management imperatives and clinical governance, will not be able to provide the conditions required for practitioners to implement new approaches to specific local challenges.
Articulating the Social Model: why is it necessary?
Clarity about the nature of the social model and it's theoretical and evidence base is necessary for four reasons. These relate to the underpinning influences and characteristics of the modernising health policy context. It is suggested that these include:
The fluidity of these developments at this point in their evolution offers a number of opportunities for embedding both the theory and the practice of the social as an integral and valued element in the arsenal of resources and structures which are being put in place to address health challenges. There are also obstacles, which, if not addressed may result in the denigration of the values and methodologies that inform social practice, to the detriment of service users, communities and practitioners. These four reasons are elaborated below.
1. Partnership: The lynchpin of new health policy
The concept of partnership has become a cornerstone of a range of recent shifts in policy aimed at modernising institutions across the whole field of civil and public life. It is one of the ten core principles for the NHS established by The NHS Plan and new partnership arrangements are a central feature of the new health and social care policy landscape. The same preoccupation with the development of effective partnership arrangements can also be discerned in, for example, the areas of crime, education, legal services, housing, regeneration and community development, skills and workforce development. Partnership is no longer an 'add-on' in policy and service development but the fundamental characteristic of the public sector modernisation endeavour.
Policies and partnership: joining things up
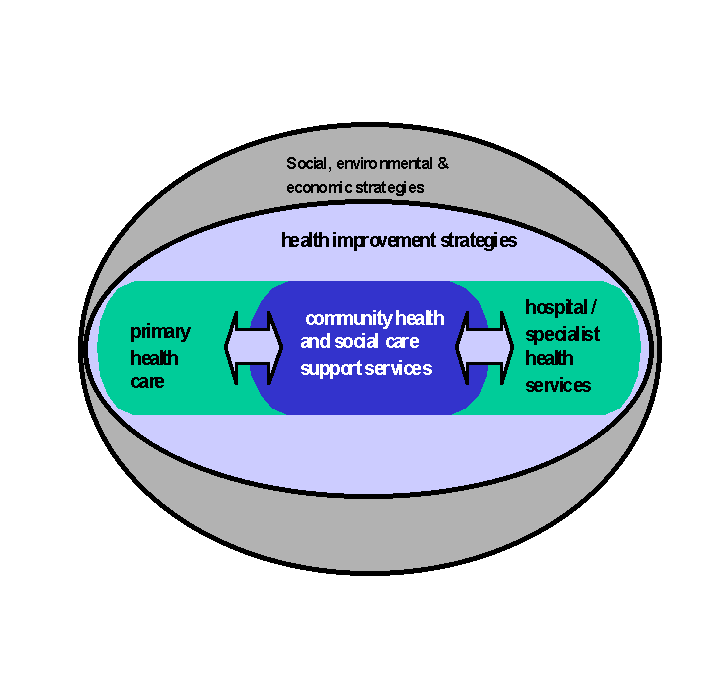
The opportunities for partnership in new health policy arise in multiple and interconnected arenas as illustrated in Figure 1. These address the areas of health and social care services for the ill and vulnerable and have already given birth to PCTs and other structures designed to improve the quality and effectiveness of these services. However, a key characteristic of the new health policy environment is its broad interpretation of the concept of health and a focus that goes far beyond the traditional 'reach' of the NHS and social services to the wider social, environmental and economic factors affecting health.

Figure 1
Partnership is no longer an 'add-on' in policy and service development but the fundamental characteristic of the public sector modernisation endeavour. In such circumstances, care needs to be taken to ensure that new partnership structures achieve powerful synergies between agencies and disciplines, in order to target resources and interventions effectively and comprehensively, whether these are at the level of individuals, groups or communities.
Towards a Unifying Theoretical Base?
An important question to be asked at this stage is whether all of the new national and local strategic drivers will, in time, simplify and link partnerships? It is clear that the government wishes to support a unifying process and has committed itself to a review of guidance to make the links clear. However even these arrangements may not be sufficient to overcome the deep -rooted political, organisational and cultural barriers that have inhibited partnership working. Evidence indicates that these are considerable barriers to the development of effective partnerships, irrespective of the requirements of new policy. It has been suggested that the environment may continue to be unconducive to partnership development when national frameworks are focused on monitoring of performance rather than development, and where the measurement of partnership success is short term. In such a context, the implementation of partnership and modernisation policy is hampered by internal blame cultures, poor change management and a failure of lateral thinking amongst key managers. As important, the lack of a shared understanding about the social nature of health itself, the causes of illness and disability and a variable commitment to prevention as well as to cure may yet prove the new policy emphasis on partnership to be an unachievable illusion in practice. Conversely clarity about all of these may provide a unifying focus for practice, which can take account of individual and community health needs and provide the range of responses, from the social to the biological that they require.
Skills for Partnership
At policy level, partnerships are attractively simple and economically sound. However partnership has other, more complex meanings at the level of individuals and communities. Clarity is required in determining what the point of partnerships is in the first place. Are they for example partnerships with service users, fellow citizens or communities? Are they with other professionals of different or similar status? Are they with other statutory organisations or the voluntary sector- or as will happen increasingly, with the private and commercial sectors? Are they about improving health, tackling crime and creating safer communities, or are they to deliver treatment and support to ill and disabled people. It has been suggested that in delivering support to people with complex needs up to fifteen boundaries may have to be successfully negotiated. Across all of these dimensions, imbalances in power, authority and resources abound and are part of the dynamics of the partnership. Navigating these will need, as a minimum, the following range of skills and knowledge:
These skills are the essence of the social approach and have particular relevance to mental health services. Moreover, as discussed here, it is clear that they are fundamental to the practice of all mental health professionals- not just those associated with social care.
Trade-offs: scientific-bureaucratic approaches versus community empowerment?
Government policy in the UK is removing organisational and financial blocks to partnership between health, social care and, more recently housing organisations and is introducing a range of new, collaborative structures to deliver the overall agenda. Some, like Sure Start, operationalise a recognisable model of social intervention aimed at empowering families in deprived areas to take more control over the conditions of their lives. Recent guidance on new Local Strategic Partnerships (LSPs) open up additional realms of possibility for the development of multi sectoral partnership approaches to neighbourhood renewal and physical and social regeneration that may have much to contribute to the improvement of mental and physical health in populations.
However, there are at the same time, indications that partnerships for delivering the traditional health and social care agenda may mean that services for people who are vulnerable or who suffer ill health and disability become much more clinically driven. It has been suggested that the modernisation process in health services is characterised by the development of 'scientific-bureaucratic medicine' reflected in clinical governance and the institutions that support it, the National Institute for Clinical Excellence (NICE), the Commission for Health Improvement (CHI). These institutions and the system they control, including the implementation of NSFs, feature increasing degrees of specification, standardisation and central control. Moreover, they are sharply at variance with models of practice, which stress the validity of personal experience, however critically examined, as the primary source of valid knowledge. Instead it asserts that valid and reliable knowledge is mainly to be obtained in the accumulation of research, conducted according to strictly scientific criteria. The dominant interpretation of these criteria is that randomised controlled trials (RCTs) provide the most valid inferences about the effects of clinical interventions and that the most appropriate means of aggregating the findings of such trials is some sort of systematic review.
The Social Care Institute for Excellence
It remains to be seen how, in the shadow of NICE and clinical governance, the new body, The Social Care Institute of Excellence, (SCIE) will operate to support an understanding of social interventions at either individual or community level. Evaluations of first wave Health Action Zones have documented a range of difficulties in finding objective measures for activities that involve:
SCIE exemplifies the potential threats and opportunities inherent in the new agenda. On the one hand it enables for the first time a high profile, sustained approach to mainstreaming knowledge and understanding in support of social interventions. On the other hand, there is a risk that it will be obliged to go down the track established by NICE, which confers high status on certain ways of knowing the world rather than others. In this context, the concept of reflective practice, which has been the dominant model of evaluating actions within the social care field represents a significant challenge for incorporation by SCIE. There is clear evidence of its effectiveness- even within clinical arenas. Even more challenging, the 'decline of deference' and the renegotiation of relationships between service users, patients and professionals requires new ways of understanding and valuing lay expertise. SCIE will need to evaluate the impact of strategies for empowerment and capacity building, as well as the outcomes for those who receive support services. This may require fundamentally different approaches. It will also need to have sufficient influence in its own right, commensurate with that of NICE, to influence the evolution of practice. However the playing field between the domain of NICE and that of SCIE is not a level one. There is currently a lack of investment in evidence that would enable the integration of social science insights into mental health services. It is to be hoped that the newly established National Institute for Mental Health will play an important role in rectifying this imbalance.
Finally, as the direction of travel is for mental health services to become more clinical it needs to be acknowledged that this is merely confirming an historical trend. Evidence suggests that collaboration between disciplines in CMHTs has been far from optimal and that, at the end of the day these teams find it difficult not to adapt their practice to the ‘lowest common denominator’- the medical model. In such circumstances, the development of Care Trusts and integrated Mental Health Trusts using Health Act Freedoms and flexibilities may mean that the skills and understandings of proponents of the social model, particularly social workers, will not be supported by the ethos of services. New mental health policy requires mental health services to address risk management and crisis resolution. Local agencies will be held to account against tight targets for implementation. Practice will increasingly be bound by clinical governance. Commissioners of mental health services will wish to see swift progress in implementing the requirements of the NSF in key areas. In such circumstances it is feasible to speculate that neither primary nor secondary prevention or community empowerment issues will be at the top of the list of priorities for the foreseeable future. These concerns are compounded by worries about the implications of the proposed reforms to the Mental Health Act.
Male Former Drug User. Age 28 years SURREY
I have had a CPN, for seven years. He was good for my medical needs, but let me down badly when it came to the rest of my life. CPNs can only work with health issues - at least that is what they did for me. My CPN got me in to detox but when I finished he left and I ended up with an ASW who really changed things for me. She took me through my whole life got me moved to a proper flat, helped me sort out furniture electric and my debts. My ASW also got me help with looking after myself, learning to cook proper meals and washing , cleaning. I still have my ASW and an OT. For the first time in years I have a proper life.
Losing or gaining ground?
These worries reflect anxiety about changes to the statutory roles of Approved Social Worker, but also disquiet about the civil liberties implications of the new proposals, particularly in relation to the proposals for the detention and treatment of those with presumed ‘dangerous personality disorder'. There is a clearly a vital need for clarity about the value and effectiveness of social interventions to support individuals and groups with mental health problems to temper and modify this process.
We worked pretty effectively for years with so-called personality disordered clients when the NHS wouldn't touch them with a barge pole because they are supposedly untreatable. We supported and contained them pretty well by negotiating boundaries for their lives, structuring their daily activities and- vitally- getting them off the streets. It didn't lead to a great quality of life all the time. These people need huge amounts of support and probably, dedicated teams. But it contained them. We've been unable to do this in social services for years and CMHTs in my experience aren't interested and wouldn't see this as part of their brief.
Social worker. CMHT. Berkshire
2. User Involvement and Citizenship
However, these concerns need to be seen in a context that demonstrates another key influence on the partnership agenda and a different direction of travel for parts of the system charged with delivering the new mental health agenda. These influences relate to ideas about citizenship and social inclusion, which have, in recent decades urged the integration of people requiring support within the general population rather than setting them apart. The social model of disability separates an individual's impairment, whether physical or mental from the social, economic and environmental factors that limit participation as citizens, including for example, inaccessible buildings and transport, blocks to education, training and employment, and lack of access to health care and social support. In relation to mental illness this has encompassed the negative social attitudes inherent in the stigmatising process. These developments have brought service users, their carers and other members of their social networks into a new relationship with services and with professionals. However, the modern social model goes far beyond the social model of disability to engage with the profound social and political changes that characterise the age.
SIRI Behavioural Health. London
The project provides holistic counselling to African and Caribbean communities. The aim is to address the presenting mental issues and also to address practical and social support issues-including housing needs, leisure, entertainment, and income maximisation. The aim is for SIRI's users to grow and develop through to independence. SIRI is self-help, user directed and user led organisation. A range of success measures have been identified in evaluations
Democracy and participation
National policy in a number of sectors urging greater attention to the rights and responsibilities of citizens to participate in protecting and promoting their own health and in shaping and influencing the priorities and delivery of public sector services. This is a medium term priority for the NHS in the context of the NHS Plan and Shifting the Balance of Power and many other key national policies. It is an explicit component of many of the seven standards established in the Mental health NSF.
These developments mark a distinct shift in health policy emphasis, away from the market- driven mechanisms proposed by previous governments. Current health policy replaces this with notions of partnership between professionals and the public. This reflects public discomfort with the notion that health care is simply another commodity to be bought and sold in the market place and evidence that the rational choice theory could not deal adequately with the reality of professional- patient relationships in conditions of uncertainty, risk and unequal power.
The current policy preoccupation with rights, responsibilities and participation has its roots in developments in contemporary social and political thought that try to understand major currents of societal change and redirect institutions away from hierarchical or market solutions to ones that are more inclusive and participatory. Anthony Giddens has argued that expertise no longer has pride of place. Where we once thought that science was the authoritative route to mastery and control, it has become clear that science also manufactures uncertainty and generates new risk. No forms of expertise can be given free reign. All can and should be questioned. Different viewpoints need to be constantly brought into contact with each other and forced to ' declare themselves'. However, even this view has been criticised as limited. It is suggested that these developments are now so entrenched and refined that we are dealing with a post-modern discourse, in which ‘lay’ knowledge is also an alternative canon of expert knowledge and should therefore be as valued as that of professionals.
Refugee and Asylum Seeker Participatory Action Research. Manchester
This project has the aim of developing long term participatory action with, rather than on, refugee and asylum seeking communities. This project sees refugees and asylum seekers as part of the solution and their involvement is central
Distrust of science
Underpinning these developments there is widespread public concern about a number of public health issues ranging across disparate areas including the BSE crisis, the debates on the introduction of genetically modified foodstuffs, concerns about animal testing and the ethics of cloning and stem cell research amongst others. This concern has, in some sections of the population become overt suspicion of the goals and values of scientific inquiry. There is increasing interest in untried and unproven alternatives. It has been suggested that there has been a profound loss of public confidence in both individual health care professionals and the service as a whole in the last two decades of the 20-Century.
These attitudes are, it is suggested, directly related to the sheer scale of technological advance, which has introduced both real and imagined fears about human culpability rather than natural disasters as the source of many risks in contemporary society. Beck's concept of the 'risk society' suggests that rather than providing the solution to all our ills, science has created new dangers about which we are only just becoming aware. It needs to be noted that the increasing risk averseness of modern society has extremely negative connotations for perceptions of people with severe mental illness, fuelling the preoccupation with assessing risk and creating ' safe' as well as sound and supportive services. It has also informed the proposals for reforming the Mental Health Act. Hence we enter a New World in which we seek to involve the austere rationalities of scientific method to guide services and strategies in some areas, but also integrate into our policy response the irrational fears of the mob.
This context requires new attention to models of professional practice and service delivery which are theoretically rigorous but which brings professionals and service users into new, more equal and more honest relationships with each orther.
This is a considerable challenge within mental health services where users and carers must, at times place their trust in professional opinion and service capacity to deliver required support when these professionals may also need to use coercive powers. Resolving these dilemmas obliges staff to have high order knowledge and skills, rooted in an awareness of the social context of interactions and an understanding of the need for and impact of empowerment strategies on individuals and communities.
FEMALE 43 YEARS (CORNWALL)
I have been in and out of mental hospitals all my life. On strong drugs, feeling like shit. I have tried to kill my-self many times. All because I was abused when I was a kid. I have a social worker She has been with me for the last three years. She looks after me in loads of ways. I don’t want to go back in to hospital again. She sees it as her Job to keep me out.
The third main influence on the rearticulation of the social model reflects the growing recognition that there are links between policies on health and those, for example on housing, the physical environment, employment and other functional areas and the need to tackle issues such as urban deprivation in a co-ordinated way. This approach holds out the prospect of confronting the longstanding, interconnected problems affecting the public's health - and in particular of reducing the health gap between social groups and tackling social exclusion - more successfully than discrete policies in specific, functional areas. The multi factorial nature of mental illness has been accepted since the late 1970s, with the publication of the groundbreaking study by Brown and Harris of the social contribution to depression in working class women. However, these insights have not yet been accompanied by sustained, systematic community based interventions to the prevention and treatment of mental illness.
Standard 1 of the mental health NSF, which focuses on mental health promotion provides a national policy framework within which to mainstream these approaches. This requires an accepted definition of the social model of mental health, the development of new skills and new interventions to address the root causes of poor mental health, including those which derive from social and environmental deprivation, racism and social roles.
Addressing health improvement and tackling health inequality
This emphasis within modern mental health policy is supported by the broad framework for health improvement as set out in the English public health white paper, Saving Lives: Our Healthier Nation and equivalents in Scotland and Wales. The white paper establishes mental health as a national public health priority. The reduction of deaths from suicide and undetermined injury by a fifth by 2010 is one of the five targets of the public health strategy.
The white paper emphasises the complex interactions between life circumstances, life events and biological risks based on a life course approach to health. This understanding enables a more holistic approach to health improvement for individuals and communities. It puts Britain in step with developments in and beyond Europe. This has important implications for practice, which are explored below.
Improving public health has always been a multi disciplinary, multi agency effort with some of the greatest improvements in health being achieved by the actions of local government rather than health professionals. However, in recent years, there has been a loss of function and vision within public health. Whereas in the nineteenth century the accent lay on public hygiene and disease prevention, in the 20th century the emphasis came to be placed on combating the diseases themselves, with less need for preventive policy. One of the less positive consequences of the scientific revolution in medicine was the sidelining of public health and its replacement by a model of health based on medicine. The dominant perspective shifted accordingly, away from a focus on the connection between human health and social environment, and onto the doctor and the hospital. Since then we have seen a strong advance in successful medical technology at the expense of investments in local health policy. The result has been that health care has become one of the most prominent features of the national budget and the 'health' of the NHS the ubiquitous topic of public attention. Planning for health has been subsumed by the need to plan - and invest - for illness and disease.
Under the previous Health of the Nation Strategy, pride of place was given to health education as a means of improving health trends while health inequalities were largely ignored. Even so, in the years following the Black Report (1980) there has been growing recognition that inequalities in health cannot be solved by the NHS alone or simply by ‘better health education’. It is clear that at the beginning of the 21st century, we need to reconnect with the roots of public health and develop approaches that impact on all the determinants of health and not just those that relate to biology and lifestyle. It is vital that developments within mental health are congruent with those established by the new public health agenda and that the value of the social model is promoted within the modernisation programme, together with the skills to implement it
However, it needs to be acknowledged that the focus on treatment by the NHS has proved to be remarkably resistant to change. Spending on prevention is still less than 1% of the overall NHS spend. As Webster notes at the conclusion of the second volume of his history of the Health Service:
‘ While the National Health Service claimed from the outset to give high priority to the promotion of health…. in reality this aspect of the service was never more than weakly developed, notwithstanding claims to the contrary, habitually made in ministerial speeches’.
This suggests that protagonists of social approaches to the prevention and treatment of mental illness should not be complacent. Notwithstanding the opportunities inherent in modern mental health policy, there is an urgent need to raise awareness about the effectiveness of social interventions, to win increased resources for further research and skill development- and as important, to gain recognition for expertise in the delivery of social interventions.
MALE 22 YEARS PLYMOUTH
I have been in and out of Hospital mostly because of drink and not taking my tablets. Life was crap. I ended up in prison for a year. I tried to kill my-self and cut-up bad in there. When I came out I got a social worker for the first time he talked my language, got me sorted. My social worker makes me feel like a person - not a mental idiot who needs crap drugs.
Health, Complexity and Interactivity: no ‘one size fits all’ approach
Recently published Canadian research sheds further interesting light on many of the issues addressed in this paper. In a review of a large number of different studies and a series on interactive events, the study takes a careful look at three questions:
The study demonstrates the complexity of each, pointing to the need for a powerful new framework for thought and action in each of these fields.
'We now realise that numerous, perhaps countless, forces from many different spheres of influence shape health, ranging from the molecular to the socio-economic.
This research urges special care in understanding the circumstances and nature of complex systems, asserting that there is no formulaic response. For a long time, medical tradition has focussed on health in terms of the living organism. Advances in medical knowledge have resulted from a better grasp of the physiology and psychology of the individual interventions attempted to prevent or cure illness in the body.
A second tradition regards the environment as more important to an individual's health than medical intervention. This idea lies behind public health initiatives like sanitation, mass vaccination and health promotion campaigns designed to alter unhealthy behaviour. Its most recent expression is in the field of population health, which identifies socio-economic factors as the source of persistent health inequalities.
The conclusions of this work suggest that there is a need for a third approach. This recognises that it is the quality of the interaction between the individual and his social context that are important for health. Negative interactions are associated with lower health status, positive interactions with higher health status. This complex notion of health entails an equally complex health policy response and new interventions that are, at root, social. This 'third way approach,' defines the nature of the new model for mental health practice.
Social Capital
In this context, the concept of social capital is relevant to the task of tackling health inequalities and social exclusion. Higher social capital, it is suggested, is implicated in a range of positive policy outcomes including higher rates of economic growth, lower crime rates, better local and national government and better public health. It is further suggested that it is a particularly valuable way of understanding the causes of the growing gap in health status between the richest and the poorest in our society and for the development of public health interventions aimed at improving the health of the poorest.
There are many different definitions of social capital in use in the literature. The concept involves social relationships, social support, formal and informal social networks, group membership, shared norms, trust, reciprocity and community and civic engagement. Putnam defines social capital as the "features of social organisation such as networks, norms and social trust that facilitate co-ordination and collaboration for mutual benefit" Social capital therefore links the individual with institutions and organisations through social and civic networks. Active participation in these networks, builds the social trust that underpins cohesiveness and collaboration, the important resources for health and health creation. Social capital therefore places a high value on co-operation, participation and social inclusion. These have also been demonstrated to have a positive impact on mental health.
Social capital has a role to play in improving and sustaining the health of the public. It can do so in three ways:
Some may argue that the link between social support, social networks, self-efficacy and good health has been known for some time. In what ways then does the notion of social capital develop our current understanding or offer a fresh perspective those interested in improving health and well being? One way of answering this question is to suggest that, if inequalities in health are, as seems to be the case, indeed driven by relative power imbalances in societies, then the concept of social capital provides one way of understanding the problem and paves the way for an approach to improving health that incorporates community empowerment goals. Effectively involving local people in shaping and influencing decision making about health and enabling sustained involvement increases social capital at local level. This has particular value in the development of strategies to overcome the social exclusion suffered by people with poor mental health.
Mann Ki Baat: Birmingham
Mann Ki Baat aims to combat the stigma around mental illness, encouraging Asian people with mental health problems to take positive steps to tackle their problems
4. Clarifying the Evidence Base
The fourth influence on the nature of the social model in the new context for mental health and health policy generally relates to the clear evidence of the effectiveness of social approaches to health improvement. The range and diversity of these is set out in a series of case studies in the LGA publication: A picture of health: an audit of regeneration of health. It is notable that the strengthening of local capacity whilst regenerating local infrastructure is a consistent feature of these initiatives.
Some of these developments demonstrate impacts on mental health amongst other positive health effects, but, to date, there has been a lack of systematic investigation into the impact of large-scale changes in socio-economic circumstances on mental health. This deficit needs to be addressed urgently.
Community Development Approaches to Health Improvement
The Report of the Health Select committee praised the Beacon Project on a housing estate in Falmouth, Cornwall, which was awarded a Nye Bevan award in 1999 for its remarkable contribution to health improvement. This project used community development approaches to bring about a range of social and environmental improvements in the poorest ward in Cornwall. As the report of the Health Select Committee says, 'the results of the project have been nothing short of remarkable:
Evidence exists in particular about the benefits of these approaches with people who are socially excluded.
Darlington Borough Council: Including Young Mothers
The Before / After group is a multi agency project involving the Department of Social Services, the Education Department and the local Primary Care Trust. The project aims to involve all local agencies in working together to meet the needs of pregnant schoolgirls who are not attending mainstream school and are not in touch with other services. The young women attend a resource centre up to five mornings per week. Teaching is provided by the local authority Home and Hospital teaching service, who provide a teacher to ensure that their educational needs are met. Social isolation is reduced with peer group support developing. The social and developmental needs of the young mothers and their children are addressed by social services and two dedicated community midwives who cross the ordinary boundaries of their service to ensure appropriate take up of ante and post natal services.
The impact of social w
ork Interventions in mental healthThere is very poor public understanding of actual social work practice in mental health, notwithstanding the considerable evidence base supporting its effectiveness. That said, social workers have not been their own best advocates. Recent research considered the evidence base of social care and confirms the view that many social workers are not considering research or evidence in their practice.
Nonetheless there is long history of the social work contribution to effective, empowerment orientated mental health interventions.
|
The Social Work Contribution to Mental Health Source: Professor S. Ramon |
More recent examples of this approach, aimed at empowering the users of mental health services are provided in the case study below.
Elmore Project. Oxford
This team operates a street outreach service. This is mainly targeted at people who have multiple needs and sleep rough, though the team also makes contact with people who spend most of their time on the streets but do have accommodation. The team adopts a needs led approach, aiming to fit the service to the multiple and complex needs of the client. There are no narrow, exclusive eligibility criteria. The aim is to spend enough time to focus on the underlying causes of the symptoms and, where possible to address social and emotional networks. Primary care and housing related services are provided. The approach has been successful in supporting street living people with mental health problems to obtain and sustain accommodation.
However, it is notable that the new legitimacy of community development and capacity building approaches has not extended to social workers- or indeed to social services departments. Increasingly, the opportunities for interventions like these described above belong to other departments of local authorities and to new health partnerships.
We want to have referrals from women who have experienced post partum depression previously, or from women who suffer antenatal depression which is a common problem. We find that the midwives don't understand depression in pregnancy and are frightened of mental health problems. They don't ask the right questions, won't use the Edinburgh Post Natal Depression Scale which, although not foolproof, is a way of detecting at risk women and so (they) don't refer. We have found that early intervention, counselling, support with making necessary arrangements like childcare is very helpful although this approach has not been well evaluated.
Conversely the midwives may refer everyone they see with a history of depression to us, even if they (the clients) don't want to be referred. There seems to be no training and limited understanding of mental health amongst the ante natal clinic staff
Social Work Team Leader/ NHS Acute Trust
Social work morale
In this context, the continuing ‘ bad press’ affecting the public image of social workers is a major problem as it distorts the discussion away from what social workers actually achieve in both preventive and rehabilitative work with individuals, groups and communities onto a small number of high profile scandals and disasters. In these circumstances, there is a danger that the social model and the social care disciplines will not be highly valued in the new mental health services. This declining status is compounded by the retreat from the preventive role of social work in recent years and a reductionist view which associates social work entirely with the administrative tasks inherent in care management and care packaging.
How do I retain good staff when there is such low staff morale? How do I keep staff moral high when clients don't get better? How do I support my staff to work with chronicity when I have to draw on agency workers all the time? There is no team ethos possible in such circumstances, no understanding?
Manager: Supported living project, London.
A
continued role for social work in mental health?The critical question is whether the promotion of the social model requires the continued existence of social work as a discipline. The evidence reviewed for this paper suggests that there is a strong case for the preservation of social work both as a repository of social science insights, analysis and methodologies and as the key vehicle for their translation into practice.
Opportunities exist now to raise the profile of the discipline with the introduction of a new degree level qualification and the General Social Care Council. Attention needs to be paid to how best to support these developments with a dedicated research and development function, capable of retaining and valuing its social work roots but able to address the modernised health and social care agenda within the overall framework proposed above. With this support social work could begin to take an equal place amongst the disciplines that currently contribute to mental health services. Social workers must lobby for equal treatment with nurses for example, who are now able to attain 'consultant' status. Is there not a case to be made for equivalent social work consultants, with sufficient status to address the training needs of increasingly multi disciplinary service settings? With the withering of organisational bulwarks, the responsibility for the preservation and extension of the social model must reside with the profession itself. The challenge might be more successfully addressed if there were clearly identifiable leaders and experts in the field, with a status commensurate with that their health service colleagues.
I manage and supervise both social work and health staff including a consultant psychiatrist. I struggle with feelings of confusion and isolation. I manage vacant posts by doing extra ASW duties myself and by supervising more staff than in my job description. I still have to fulfil the duties of middle manager, implementing the NSF and risk assessment procedures, finding creative ways to incorporate care management with the CPA- all with outdated computer systems. There is huge anxiety within my so-called team.
CMHT Manager: Surrey
This does not mean taking a regressive stance. Social work will clearly have to move with the times. This may mean severing the link with departments of
social services and moving confidently into new, multi disciplinary service formations. There is a vital need to ensure that the new cadre of social work leaders has the management skills for the new agenda.
The Question of Evaluation
It is clear that the promotion of a more holistic understanding of health needs to be bolstered by the development of an appropriately wide but related set of indices. This would introduce a broader understanding of health outcomes. Much is known about death, disease and hospital utilisation. This must be complimented by data on functional ability, disability and well being since these are key health outcomes also. We also require valid and sensitive indices of the health of our physical and social environment. Some of these exist already (air quality, traffic data, housing surveys) nonetheless many gaps remain (e.g. views of individuals and communities, indices of the social environment.) More importantly most of these indices have been developed in isolation and are not examined as a whole. These indicators should not be seen as targets as such, but as indications of change towards holistic health policy. The Local Government Association (LGA) points out in its Regeneration and Health Audit that area regeneration takes a long time and there is a need for intermediate and process markers to ensure that progress is in the right direction. As discussed above, the current policy emphasis on 'scientific-bureaucratic medicine' may not be the most appropriate approach for evaluating the impact of the social model.
In spite of these challenges there are numerous examples of the ways in which attempts are being made to develop methodologies for measuring the impact of their activities in relation to health improvement.
Dumfries and Galloway Council: A Participative Community Health Needs Assessment
The Dick's Hill Pathfinder Community Development project has undertaken an innovative community health needs and quality of life assessment involving the local community. This was used to supplement existing quantitative data about local health and socio-economic variables.
The primary method used to generate the qualitative data was the use of focus groups within a community development framework. Although not a new technique as such, the novel element in this activity was the way in which representative groups of local people, including children and young people, were 'sampled' and invited into the focus groups.
The focus group methodology was found to be a form of community participation in its own right. The research process has generated interest, good will and enthusiasm within the community. It also provides a useful snapshot of the strengths and weaknesses of local services and of the aspirations of local people and the obstacles to their achievement. A wide range of recommendations has emerged from the initiative to inform the regeneration programme in Dick's Hill.
|
Calderdale MBC: Health Needs Assessment Calderdale MBC has been awarded Beacon Council status for Local Health Strategies. It has a clear vision for improving health and was commended for demonstrating how results can be achieved by removing barriers to effective joint working with health partners. In 1999 a range of health and independence indicators were introduced. A local multi-agency group, involving the council, Primary Care Group, Healthcare Trust and Health Authority, developed some 90 indicators. They are crucial to the HImP to identify the health needs priorities for the population and also give a baseline for change and monitor progress towards achieving the overall goals of improving the health of the population as a whole and improving the health of the worst off in society. Calderdale Council worked closely with the NHS to benchmark the health profile of the local population. Health Needs Assessment methodology and an operational model has been developed and used to inform a performance management regime which identifies ’health gains’ and reductions in health inequalities. |
Conclusions: the nature of model
What then is the nature of the model that is being proposed in this paper in the context of the policy shifts, underpinning theories and emerging evidence which have been summarised?
The Modern Social Model in Mental Health: essential characteristics
The modern social model in mental health has the following key characteristics:
Endnote:
The integration of approaches based on the social model carry with them radical implications for the education and training of mental health practitioners- and for the ethos of service and performance management frameworks. Some of these are very robustly addressed in recent work and are not summarised in this paper. There is also a critical need to invest in a new research agenda in mental health to test social interventions, which would include system level and individual alternative approaches. Without this there is no systematic defence to the dominance of the medical model, bolstered as it is by the scientific - bureaucratic imperatives and structures of the new NHS.
In these circumstances, there is a danger that the social model and the social care disciplines will not be highly valued in the new mental health services. In order to overcome these difficulties, there is need to clarify the evidence base and to assertively promote it. At the same time, there may be a need to move with the times and allow new roles to emerge to deliver effective, high-quality, social interventions within multi disciplinary teams in new organisational contexts. This paper has attempted to define the characteristic of an approach to delivering the new mental health agenda that integrates the insights and understandings that influence broader health policy.